WARNING!! The information and photographs contained in this guide are quite explicit and may be disturbing to some viewers. By entering our site, you agree that you are either an adult, or have your parent or guardian’s permission to view explicit information and images on the internet. Please review our user agreement and medical disclaimer before going any further. IN NO WAY SHOULD AFRAIDTOASK.COM’S SITE OR ONLINE GUIDES BE CONSIDERED AS OFFERING MEDICAL ADVICE!
Welcome to AfraidToAsk.com’s Contraception & Birth Control Guide. This guide has been developed to help you learn about common contraceptive methods and to make informed decisions about your health and life. Though this guide is a good start, we strongly recommend you call your own doctor or a local family planning clinic to take the next step in learning more about correct contraceptive use.
The probability of pregnancy after a single act of intercourse is calculated to be 15% if it occurs once a week and increases to 33% if it occurs every other day. Each year 3.2 million unplanned pregnancies occur as a result of no use, misuse, or malfunction of contraceptive methods. This often poses great emotional and financial distress to the people involved, including the parents (whether wed or unwed), the unplanned child, and sometimes even society as a whole. This makes contraception and its methods a topic that must be addressed. Our goal here is to give you a easy-to-understand, yet thorough, guide to preventing unwanted pregnancies. This guide will address the family planning concept and how contraceptives actually work in preventing pregnancy. One of the best resources for learning about contraceptive choices and getting a contraceptive is your primary care physician.Another note, though this guide is focused as a contraceptive guide for heterosexual vaginal sexual intercourse, the sexually transmitted disease (STD) portions of this guide is applicable to all sexual acts, including vaginal, oral, and anal intercourse. Whether participants are heterosexual, homosexual, or bisexua, sexually transmitted diseases do not discriminate. To see detailed information and photographs about the common sexually transmitted infections, visit our STD Online Guide.
ANATOMY/PHYSIOLOGY
The sexual organs of both men and women are centered in and around the pelvis (it’s like a large bony “bowl” which includes the hip bones).
FEMALE ANATOMY
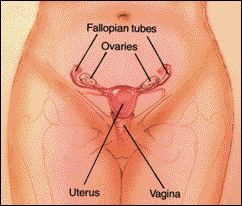
A woman’s outer genital area is called the vulva. The vulva includes the mons (the area over the pubic bone which is covered by pubic hair), the labia majora (“outer lips”), labia minora (“inner lips”), the clitoris, the openings of the urethra and vagina, and the perineum (area between the vagina and the anus). A woman’s inner reproductive organs include the two ovaries, the two fallopian tubes, the uterus, and the vagina. The ovaries are almond-sized organs and are located one on either side of the uterus. Between the two ovaries, one mature egg is released during each normal menstrual cycle. The ovaries also produce hormones, including estrogen and progesterone. The Fallopian tubes are two delicate muscular tubes which are attached to the upper corners of the uterus, one on either side. They end in little “fingers” which encircle their respective ovary. When an egg is released from the ovary, the “fingers” catch the egg and propel it up the tube towards the uterus. Fertilization usually occurs in the fallopian tube, and the fertilized egg takes about three days to travel to the uterus and implant itself in the uterine lining. The uterus is a small muscular organ roughly the size and shape of an upside-down pear. It has an inner cavity whose lining, called the ENDOMETRIUM, is rich in blood vessels. This lining builds up, matures, and sheds over the course of a woman’s monthly menstrual cycle. The biological purpose of the lining is to serve as rich “soil” for a fertilized egg to “plant” itself in. If no such egg “plants” itself, the lining is shed during the woman’s “period”. If a fertilized egg has planted itself, the lining is not shed at the end of the cycle, and the woman “misses her period”. A pregnancy has happened. The bottom of the uterus, also called the “neck” or the “cervix”, is the opening to the uterus which protrudes into the vagina. The vagina, or the “birth canal” is a muscular tube which is about 4-5 inches long which extends from the opening of the uterus to the outside world. One end opens to the outside just below the urethral opening (where urine exits the body). To learn in more detail about the female reproductive organs, please visit the Female Breast & Genital Guide. In order for conception to happen, the egg must be fertilized by a sperm. In order for the conception to become a normal pregnancy, the fertilized egg must successfully implant itself in the lining of the woman’s uterus. Preventing one or the other of these two events forms the basis of all contraceptive techniques.
MALE SEXUAL ANATOMY
The most obvious genital structure in men is the penis. The penis contains erectile tissue which fills with blood and becomes stiff and erect when a man is sexually aroused. The scrotum is the pouch of skin which hangs beneath the penis. This pouch contains two testicles. Each testicle produces sperm and the hormone testosterone. During ejaculation, sperm and substances secreted by other glands mix to form semen, which is propelled through the urethra and out of the penis. On average the average ejaculation contains 200 million sperm. The force of the stream of semen and the numbers of sperm help the chances of a sperm to travel into the cervix and upwards into the uterus and fallopian tubes, where it will penetrate and fertilize the waiting egg. To learn in more detail about the male reproductive organs, please visit the Male Genitalia Online Guide. An egg is viable (able to be fertilized) for 24-72 hours after it is released by the ovary. A sperm is viable for about 24 hours after ejaculation. Therefore the time window for fertilization is quite wide.
CONTRACEPTION TECHNIQUES
The word “contraception” roughly translates into “avoiding conception” of a child. Some contraceptive methods work by preventing the man’s sperm from penetrating the woman’s egg (e.g., barrier methods such as condoms and diaphram), while other hormone-based contraceptives work by preventing the woman’s ovary from releasing an egg at all during her menstrual cycle (e.g., the Pill). Of course, the only contraceptive method which provides fool-proof protection against pregnancy AND all sexually transmitted diseases is abstinence. The goal of most contraceptive techniques is to prevent sperm from fertilizing an egg. This event can be prevented by: * not engaging in sex practices where semen could contact the vagina in any way. * preventing the ovary from releasing an egg by hormonal treatment (e.g., The Pill, Norplant, Depo-Provera) * preventing sperm from entering the vagina (e.g., condom, vasectomy) * preventing sperm from entering the cervix (e.g., diaphragm, cervical cap, sponge) * killing of sperm in the vagina (e.g., spermicidal foam or gel) * preventing sperm from fertilizing the egg (IUD (intrauterine device)) Even with the most careful use, any method can potentially fail (except true abstinence). Abstinence doesn’t necessarily mean taking holy orders, and you don’t have to be a virgin to do it. People may choose to abstain from sexual intercourse or activities where semen can contact the vagina for a time. This time can be days, weeks, months, years, or certain days each month (rhythm method). In the meantime, they may choose to engage in other activities like kissing, touching, hugging, heavy petting, mutual masturbation (with no contact between the genitals and ejaculation well away from the partner), solo masturbation, or oral-genital stimulation. Keep in mind, however, that although the risk of pregnancy is zero, getting a sexually transmitted infection (STI, STD) is possible with activities where the genital regions or secretions of one partner come in contact with some part of the other partner.
ABSTINENCE
Abstinence doesn’t necessarily mean taking holy orders from God, and you don’t have to be a virgin to do it. People may choose to abstain from sexual intercourse or activities where semen can contact the vagina for a time because of personal beliefs, religious beliefs, safety concerns about pregnancy and sexually transmitted diseases (STDs), or simply because it just makes sense to them at a particular time in their life. Remaining abstinent from sex may include any and all sexual activities (e.g., kissing, touching, oral, vaginal, anal sex, masturbation, etc.), or may just be with regards to actual intercourse; there are no set rules (unless your abstinence is based on your religious beliefs.) As such, people abstinent from sex may choose to engage in other activities such as kissing, touching, hugging, masturbation (solo or mutual) with no intercourse and ejaculation well away from the vagina. Although the risk of pregnancy is essentially zero with abstinence, contracting a sexually transmitted disease is possible with activities where the genital regions or secretions of one partner come in contact with some part of the other partner. Even skin to skin contact can transmit STDs (e.g., crabs, herpes, venereal warts, molluscum). See our STD Online Guide for more information on these and other sexually transmitted infections. It’s perfectly normal and okay not to have sexual intercourse. It may feel like everyone else out there is having sex all the time, but they’re really not. People have a wide range of sexual expression ranging from touching, hugging and kissing, to heavy petting, to sexual intercourse. Analyze your own feelings. Is this something you really want to do for yourself, or just to please your partner? Are you being overtly or subtly pressured into having sex of any kind just to keep the relationship intact? Remember that you are in charge of your own body; don’t let anyone pressure you into something you may not be ready for. If your partner truly cares for you, he or she will respect you. And don’t forget you can remind them of that fact!
BARRIER METHODS

Barrier methods rely on setting up a barrier or physical separation between the sperm ejaculated from the man and the egg released by the ovulating woman. These methods set up the barrier within the vagina and serve to stop sperm from entering the opening of the cervix (the os), beyond which the egg may wait. Barrier methods prevent contact between any sperm and the egg (it only takes one out of the millions of sperm in each ejaculate to fertilize an egg and lead to a pregnancy). It is crucial to note that the effectiveness of these barrier methods is significantly improved by the use of spermicides. In fact, one should always use a spermacide in addition to these methods below (some condoms already come with spermicide added). The most common barrier methods are as follows:
CERVICAL CAP

History:
A cap to cover the cervix is an old idea which also lead to the diaphragm. In early civilization, beeswax and opium resin was used to shape a cap to cover the cervix thereby preventing unwanted pregnancies. It has been reported that Cassanova cut lemons and limes in half to use as a cervical cap. The citric acid was believed to be a spermicide. Since the early 1900s, the cervical cap has been made from latex rubber.

How it works:The modern day cervical cap is a barrier contraceptive that blocks the passage of sperm through the cervical opening. The device is thimble-shaped and made of latex rubber and has a firm rim when compared to the diaphragm. It fits snugly over the cervix and is held in place by suction and support of the vaginal wall.Cervical caps are smaller and fit more tightly to the cervix than does a diaphragm. Cervical caps can remain in place for up to 2 days without additional applications of spermicide, though some experts believe there is a small risk of Toxic Shock Syndrome. The cap remain in place for 8 hours after intercourse.
Who Should and Should Not Use It: Cervical caps tend to be more effective in women who have not given birth in the past. One study showed that even with correct use, women who have given birth have a nearly a 25% chance of getting pregnant in a year with the cap. Other people who should avoid this method of contraception include those with active vaginal infections, an unusually short (or long) cervix, or history of abnormal pap smears.
Summary of the Cervical Cap
| Effectiveness (Failure Rate) | Typical Use: 20 pregnancies/100 women/year (80% effective) Perfect Use: Use 9 pregnancies/100 women/year = 91% effective |
| Benefits | Essentially no side effects (unless allergic to all spermicides) Does not affect hormones Don’t have to rely on the male partner Can be left in place for up to 48 hours, allowing spontaneous protected coitus Smaller than a diaphragm Less spermicide is used than with the diaphragm (allowing more pleasant oral sex) |
| Risks | Still no real protection against STDs (spermicides may prevent some STD transmission) If you don’t remember to use it on or bring it with you, it’s useless Somewhat more difficult to place and remove than diaphragm Can be disloged from cervix during intercourse Latex-allergic people should use non-latex caps, if available Theoretical risk of Toxic Shock Syndrome (2 – 3 per 100,000) for all women using vaginal barrier methods (diaphragm, cervical cap, sponge, female condom) |
| STD Protection | Poor to none though spermicide may kill some STDs |
| How to Get It | Your doctor must prescribe it. More information on this method is available from the manufacturer. |
| Cost | Initial Cost: $50 to $150, depending on ones health insurance coverage Ongoing cost: spermicide (averages to about 25 cents per coital act) |
DIAPHRAGM

History: The diaphragm has been used for contraception since the early 1900s in Europe, and shortly thereafter in the United States. Design and comfort improvements have been made in the past century, but the basic concept remains the same.
How it works: The diaphragm is a dome-shaped rubber cup with a flexible rim. The woman applies spermicide cream or gel on the inside of the cup and inserts it into her vagina with her fingers so that it fits snugly over her cervix. After intercourse, the diaphragm MUST be left in place for at least 6 hours. It should not be worn for more than 24 hours, however, because of the risk of Toxic Shock Syndrome.

A diaphragm provides effective contraception for 6 hours at a time’after that, the diaphragm must be removed and cleaned. It can then be prepared with spermicide and reinserted before having intercourse again. When not in use the diaphragm is stored in a plastic carrying case. Diaphragms are reusable and are not disposable. It is recommended that they be replaced every two years or so. Like other contraceptive methods, the diaphragm can be used during a woman’s period. A diaphragm must be prescribed by a doctor as it must be fitted to each individual woman’s unique anatomical size and needs. There are four types of diaphragms, and they come in a variety of sizes. Precise fitting is important’too tight a fit may cause discomfort; too loose may allow sperm to enter the cervix and result in pregnancy.
Who Should and Should Not Use It: A diaphragm requires the presence of mind and commitment to remember to use it before sex. Women who have frequent “unplanned” sex, who have sex three or more times per week, who are younger than 30 and who have had contraceptive failure in the past are more likely to get pregnant with this method. You must also be comfortable with inserting your fingers and the device deep into your vagina in order to properly use this device.
Summary of the Diaphragm
| Effectiveness (Failure Rate) | Typical Use: 20 pregnancies/100 women/year (80% effective) Perfect Use: 6 pregnancies/100 women/year (94% effective) |
| Benefits | No side effects (unless allergic to all spermicides) Does not affect hormones Don’t have to rely on male partner Possible lower risk of cervical cancer (controversial |
| Risks | Still no real protection against STDs (spermicides may prevent some STD transmission) If you don’t remember to use it on or bring it with you, it’s useless Latex-allergic people should use non-latex diaphragms Small risk of Toxic Shock Syndrome (2 – 3 per 100,000) for all women using vaginal barrier methods (diaphragm, cervical cap, sponge, female condom) |
| STD Protection | Poor to none though spermicide may kill some STDs |
| How to Get It | Your doctor must do a fitting and then prescribes it. |
| Cost | Initial Cost: $50 to $150, depending on ones health insurance coverage Ongoing cost: spermicide (averages to about 25 cents per coital act) |
FEMALE CONDOMS
History:
The female condom is a recent invention. The Reality condom is currently on the only one on the market.
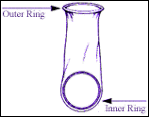
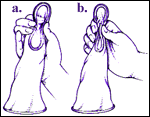
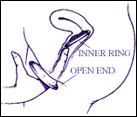
How it works: The female condom is a soft, loose fitting tube made of polyurethane. It is 7.8 cm in diameter by 17 cm long, and has a soft flexible polyurethane ring on either end. The closed end is inserted into the vagina and anchors the condom; the other ring remains outside the vagina. The external part of the condom protects some of the woman’s vulva and part of the base of the penis during sex. The inside of the condom is coated with nonspermicidal lubricant, and the condom comes with extra lubricant to use on the outside. Each condom can only be used once, and is then thrown away. It can be inserted up to 8 hours before intercourse. The female condom should NOT be used together with a male condom as both devices may then slip off. The polyurethane material of the condom is thinner than the latex of male condoms, but is less likely to tear or break. Unlike latex condoms, the female condom can be used with oil-based lubricants. Couples in the FDA study of female condoms liked the device and half would recommend it to friends. Only 7-8% of men and women did not like it.
 |
 |
 |
Who Should and Should Not Use It:
If you are uncomfortable with inserting the condom into your body, or may have trouble remembering to have it around before sex, this may not be a good choice for you. You must be comfortable with inserting your fingers and the device deep into your vagina in order to properly use this device. Otherwise, this is an excellent choice especially for non-monogamous women or women who need protection against STDs, because this method protects against STDs even better than male condoms. Anyone at risk for an STD, with multiple sex partners, or who may be in a non-mutually faithful relationship should use a male or female condom for their own protection.
Summary of the Female Condom
| Effectiveness (Failure Rate) | Typical Use: 21 pregnancies/100 women/year = 79% effective Perfect Use: 5 pregnancies/100 women/year = 95% effective |
| Benefits | STD protection includes external genitalia protection Low Cost Available without prescription |
| Risks | If you don’t remember to use it on or bring it with you, it’s useless Theoretical risk of Toxic Shock Syndrome (2 – 3 per 100,000) for all women using vaginal barrier methods (diaphragm, cervical cap, sponge, female condom) |
| STD Protection | Very good and second only to abstinence |
| How to Get It | Available over-the-counter at pharmacies and markets. The only brand currently available is Reality |
| Cost | $1 to 3 per female condom |
HORMONAL METHODS
These methods rely on giving hormones to “trick” the female body into thinking it is already pregnant so that the ovaries will not release eggs.
To understand how these methods work, here is a brief look at a woman’s menstrual cycle. During each cycle, the lining of the uterus builds up and matures under the influence of estrogen and progesterone. If no fertilized egg is implanted, the lining sheds during the “period”, when levels of these hormones drop. After the period, hormone levels begin to rise, and the lining begins to build up again. Each menstrual cycle lasts from the first day of the “period” to the first day of the next “period”. The length of each cycle is usually 28 days, but can vary widely among women and even from period to period from 17 days to 55 days. A period, or menstrual flow, usually lasts 3 – 7 days. About 14 days before the onset of the next period, and not necessarily halfway through the cycle, an egg is released from an ovary. This event, ovulation, is triggered by a rise in a particular hormone. This means that if a woman’s total cycle length is only 17 days (instead of the most common 28 days), she could potentially ovulate during her period and could conceive while menstruating.
NORPLANT

History / How it works: Norplant is a recent invention which provides five years of continuous, highly effective contraception. It is a set of six tiny tubes inserted under the skin of the arm. Each tube contains a progestin called levonorgestrel which is slowly released and suppresses ovulation. It can be reversed at any time by removing the implants.
Who Should and Should Not Use It: You may not be able to use this method if you have a previous history of breast cancer, stroke, heart disease, are taking seizure medication, or have advanced diabetes, or if you have bleeding from your vagina apart from your period. If you do not want to get pregnant for the next five years, this is a great choice. Often used by teenagers and women with many children for this reason. Excellent choice for women who have trouble remembering to use or using contraceptive methods at the time of sexual intercourse the same advantage as Depo-Provera, but more long-term. In the fifth year of use, the Norplant set is replaced. Women who are on anti-seizure medicines should use a back-up contraceptive method with Norplant at all times because anti-seizure medications can cause Norplant to fail as a contraceptive. Also, women who are taking INH therapy for tuberculosis/exposure will have the same problem.
Summary of Norplant
| Effectiveness (Failure Rate) | Typical Use = Perfect Use = 5 pregnancies per 1000 women per year = 99.5% effective |
| Benefits | See benefits for Depo-ProveraGenerally well-tolerated in terms of side effects Can be removed at any time regardless of your ability to pay for removalCheaper in the long run over 5 years of use |
| Risks | Insertion and removal both require a minor surgical procedure Norplant removal can be technically challenging Higher risk of pregnancy at the end of the fifth year High initial cost unless you have Medicaid Insurance Small risk of irritation at implant site |
| STD Protection | Absolutely none |
| How to Get It | A prescription is needed. Visit your doctor or health care provider to see if this is right for you. |
| Cost | Total cost of insertion/visits: $500-700Medicaid recipients: fully coveredNorplant Foundation (1-800-760-9030) will provide free implants and removal certificates to women who do not have Medicaid but cannot afford to pay for Norplant. |
THE PILL (OCP)
History: Also known as the oral contraceptive pill (OCP), the birth control pill was developed in the late 60’s and played a key role in the Sexual Revolution. The Pill contain synthetic either estrogen and progesterone or progesterone alone (the progesterone only or minipill). Estrogen and progesterone are hormones naturally produced by the ovaries. One pill is taken every day.
How It Works:
As you recall, a woman’s hormone levels rise and fall in the course of her menstrual cycle. These changing levels allow the release of an egg. Taking the Pill at a certain time every day without fail keeps these hormone levels at a steady level, and no egg is released. The “certain time every day” part is important as this is what keeps the levels very steady. A pack of OCPs will usually contain 28 pills – one per day. The first 21 pills contain hormones. The remaining 7 pills are placebo pills which contain no active ingredients and/or iron. During these last 7 days of a pill cycle, the woman will menstruate (usually 2-5 days) due to the drop in hormone level in the blood. After the 7 days are over, the woman starts with a new pack.A woman can start taking the Pill on a certain day (usually Sunday) immediately after her menstrual period, or on any Sunday. If she starts just after her period, she will theoretically be protected against pregnancy from day one, but should still use a back-up method (condoms and foam) for the first week (though some doctors suggest using a back-up method the entire month). If she starts on any Sunday, she will not be fully protected against pregnancy for the first month and should definitely use a back-up method during the first month of pills.There are many types of OCPs; your doctor or health care provider can help choose the right one for you. The most common pills prescribed are the low dose (lower levels of hormones) pills such as Ortho-Novum 1/35 or 7/7/7, Triphasil, Lo/Ovral, Tri-Levlin,and many others.
Common Questions:
What if I miss a dose?
Doctors generally recommend that if you miss one pill, you should take the missed pill as soon as you remember, and take the next pill at the usual time, AND USE A BACKUP METHOD (e.g., condoms + spermicide) FOR the remainder of your cycle. If you miss more than 1 pill, you should consult your doctor for advice on how to proceed. If you miss a pill AND miss a period, you may be pregnant. Go see your doctor for a pregnancy test.
What if I want to get pregnant after stopping the Pill?
Almost all women can get pregnant within a year of stopping the pill. Most can get pregnant within a couple of months.
Does the Pill increase my chances of breast cancer?
This has not been conclusively proven and most experts fell the pill will not increase your risk of future breast cancer unless you have a previous history of breast cancer. (The pill has been shown to reduce your chance of ovarian and endometrial cancers.)
Who Should and Should Not use it:
- DO NOT use the Pill if you are over 35 and smoke, even if you are trying to quit. Though the actual risk is low, smoking and the pill can be a deadly combination and women who do both are at a relatively high risk of developing blood clots in their veins which can travel to their heart and lungs and cause sudden death! Even woman younger than 35 years old can die this way, so be sure your doctor knows you smoke if you are on the pill.
- If you have a personal or family history of blood clots, stroke, heart or liver problems, strong family history of breast cancer, unexplained bleeding from your vagina, or migraine headaches, tell your doctor before you start on the pill. Though most people with this medical history can take the pill, it is important for your doctor to know and inform you of the potential risks.
- If you have a hard time remembering to take medications, don’t choose this method, because you may forget to take this too!
- IMPORTANT: If you are taking the pill and have difficulty breathing, chest pain, leg pain, headache or eye problems, see your doctor right away.
Summary of The Pill
| Effectiveness (Failure Rate) | Typical Use Rate : 3 pregnancies per 100 couples per year (97% effective)Perfect Use Rate: 0.1-0.5 pregnancies per 100 couples per year |
| Benefits |
Very high rate of effectivenessMay help discomfort associated with periods-less cramping, lighter flow, more regular periods
Decreases risk of ovarian and endometrial cancer Lower incidence of benign breast cystsMay decrease incidence of acne/ excess facial hair |
| Risks | No protection against Sexually Transmitted Diseases (STDs) Common side effects: nausea, breast tenderness, breakthrough bleeding (usually clear in 3-6 months) Serious side effects possible: Older smokers should not use the Pill (talk to your doctor) Weight gain possible Antibiotic use may decrease effectiveness of pill use backup method! |
STD Protection: Absolutely none.
How to Get It: OCPs must be prescribed and your doctor or health care provider must review your medical history to make sure OCPs are a safe choice for you.
Cost: About $20 per monthly pack. $240 per year plus cost of annual doctor’s exam.
THE SHOT
History: Depo-provera (depomedroxyprogesterone or DMPA) is a progestin-only hormone injection given every 12 weeks (three months) and prevents ovulation. Approximately 1- 2% of US women select this option. The progestin hormone is released from the muscle into which it was injected, and suppresses levels of two other hormones involved in ovulation, namely FSH and LH. It is highly effective.
How it works: Progestins prevent pregnancy in many ways. They inhibit ovulation, reduce sperm entry into the uterus by thickening and reducing cervical mucus, cause a thinner uterine lining, reduce the ability of the fallopian tube’s “fingers” to catch the egg.
Who Should and Should Not Use It: This is a great method for women who want long-term birth control lasting for three (3) months at a time, without the hassle of taking pills each day. It is also convenient for women who have frequent sexual intercourse. It is safest for those with a monogamous relationship. Because it gives excellent protection against pregnancy, people with more than one partner or with a partner who may not be faithful may be lulled into not using condoms to protect against STDs. Therefore, it may give a false sense of security. While you may not get pregnant, you may get or give HIV. You may not be able to use this method if you have a previous history of breast cancer, stroke, heart disease, are taking seizure medication, or have advanced diabetes, or if you have bleeding from your vagina apart from your period.
Summary of Depo-Provera
| Effectiveness (Failure Rate) | Typical Use 3 pregnancies per 1000 couples/year (99.7% effective) Perfect Use 3 pregnancies per 1000 couples/year (99.7% effective) |
| Benefits |
Highly effective long-term contraception Decreased menstrual cramps, minimal spotting or no periodsNo estrogen—safer for smokers (unlike the Pill)Decreased risk of endometrial and ovarian cancer Confidential means of contraception No decreased effectiveness with antibiotics
|
| Risks | Side effects include weight gain (average of 16 pounds over 5 years), breast tenderness, depression, irregular bleeding, loss of periods, and decrease in bone density.Side effects may continue until 6 – 8 months after last injection After stopping Depo-Provera, you may not be able to get pregnant for 6-12 months.HDL cholesterol (good cholesterol) levels fall with use Possible immediate allergic reaction to injectionLong term use may cause decreased bone density and osteoporosis, especially in smokers |
| STD Protection | Absolutely none. |
| How to Get It | Visit your doctor or health care provider to see if this is right for you. A prescription is needed. |
| Cost | About $35 per injection–$140 per year plus cost of annual doctor’s exam. |
IUD
History: In the 1970s, the IUD was widely used in the US (10% of all women using contraception) until problems such as pelvic infections and deaths led to some devices being taken off of the market. Modern IUDs are good, safe, long-acting and cost-effective when used in the right patient populations.
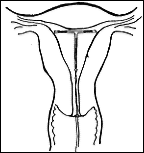
How it works: The IUD is a T-shaped device that comes with one of two active ingredients: copper or progesterone-containing. It is inserted into the uterus through the vagina by a physician and remains there for ten or fewer years. A string attached to the base of the T shape allows easy removal. Intrauterine devices are believed to work by preventing a sperm from fertilizing an egg. In the case of the copper IUD, copper ions in the uterine and tubal fluids are believed to prevent fertilization of the egg. Studies show that copper IUDs actually prevent fertilization of an egg and not implantation of a fertilized egg although theoretically this is possible (and is the common belief of how they work). The progesterone IUD works hormonally by preventing ovulation and thickening the cervical mucus to prevent sperm from entering the uterus. The copper IUD can be used for up to 10 years; the progesterone IUD can be used for 1 year.
Who Should and Should Not Use It: This method is especially good for women in mutually faithful relationships, who have had at least one child, and are interested in reversible, long-term contraception. Women who are allergic to copper, who have sexual transmitted diseases (STDs), who have more than one sexual partner, who have had pelvic infections, who have fibroids or abnormal uteruses should not use IUDs as the risk of complications and infections goes up significantly.Women who have not yet had children should avoid using IUDs as there is a higher incidence of certain complications. IUDs are not recommended for women who are taking steroids, have HIV or AIDS, have unexplained or abnormal vaginal bleeding, have cancer of the cervix or uterus or abnormal pap smears. Women with a history of breast cancer or a suspicious breast lump should not use the progesterone IUD, and should alert their doctor to the lump.
Summary of Depo-Provera
| Effectiveness (Failure Rate) | COPPER IUD Typical Use: 2 pregnancies per 100 women per year (98% effective) Perfect Use:1.5 pregnancies per 100 women per year (98.5% effective) Progesterone IUD Typical Use: 8 pregnancies per 1000 per year (99.2% effective) Perfect Use: 6 pregnancies per 1000 per year (99.4% effective) |
Benefits
Protection for up to 10 years
Ease of use
Women who can’t use hormone methods can use the copper IUD with good protection
Risks Increased incidence of PID (pelvic inflammatory disease) which can lead to infertility and internal scarring
Higher risk of contracting HIV and other STDs if other protection not used
2-10% of users spontaneously expel the IUD from their uteruses in the first year
Though risk of pregnancy is lower than most other forms of contraception, there is a higher risk of ecotopic pregnancies if one gets pregnant while using an IUD (ectopic pregnancies are a medical emergency).
Risk (1/1000) of injury to uterus during insertion of IUD; commonly insertion causes cramping and discomfort. STD Protection Absolutely none. (May actually increase risk of contracting HIV and other STDs.) How to Get It Visit your doctor or health care provider to see if this is right for you. A prescription is needed. Cost About $150-200 for the total cost of IUD plus insertion and exam
RHYTHM METHOD
History / How it works:
Although the rhythm method can work for some couples, the human body and its cycles can be unpredictable. This method operates on the premise of predicting ovulation by charting the woman’s temperature at a certain time daily over several menstrual cycles and/or analyzing cervical mucus quality and thickness. Intercourse is then avoided around the time of predicted ovulation. You may need to see your doctor or buy a book on the subject to effectively use this method.
Summary of Rhythm Method
| Effectiveness (Failure Rate) | Effectiveness unknown, but at best is only 75% |
| Benefits |
Better than nothing at allInexpensive and requires no supplies
|
| Risks | Unreliable – depends on ovulation. Depends on cooperation of male partner during abstinence periods Be prepared to get pregnant and possibly catch a sexually transmitted disease |
| STD Protection | Absolutely none. |
| How to Get It | |
| Cost | Free |
STERILIZATION
History / How it works:
These methods are essentially permanent and should be considered irreversible. If you might, at any time in the future, desire to have children this is not the method for you. (That said, sterilization reversal procedures are performed with fair to good success rates for those who have later changed their minds.)These techniques require invasive procedures to complete. Both operations (tubal ligation for women, vasectomy for men) are surgeries and carry risks associated with surgery (infection, bleeding, other surgical and anestesia complications).
Summary of tubal ligation (female sterilization)
|
||||||||||||
Summary of vasectomy (male sterilization)
|
WITHDRAWAL METHOD
History / How it works:
The man withdraws his penis from the woman’s vagina before ejaculation.
Summary of Withdrawal Method
| Effectiveness (Failure Rate) | Reportedly to be 79% effective, but statistical sample may not be adequate (e.g., likely is less effective in general population) |
| Benefits |
Better than nothing at all
Inexpensive and requires no supplies |
| Risks | Requires great self-control on the man’s part Man must be able to predict exactly when he is going to ejaculate and therefore is difficult in men who ejaculate prematurely Even when penis is withdrawn before ejaculation, pre-ejaculate often contains spermBe prepared to get pregnant and possibly catch a sexually transmitted disease |
| STD Protection | Absolutely none. |
| How to Get It | |
| Cost | Free |
EMERGENCY CONTRACEPTION
History:
Originally developed in the 1960s as treatment for rape victims, this method has been improved upon over time and continues to have active research. Though it has no effect on preventing STDs / STIs, it is a second chance to avoid an unintended pregnancy. (The chance of getting pregnant after intercourse is calculated to be between 2% and 30%.) Emergency contraception methods can use by women to prevent pregnancy after intercourse in the case of unused contraception (e.g., sexual assault, forgot to use contraception) or contraception failure (e.g., condom breakage, IUD expulsion, etc). Emergency contraception methods are not as effective as the contraceptive methods listed previously; the true effectiveness is unknown but is estimated to be above 80% if used within 72 hours from intercourse. Because of side effects (nausea, vomiting, heavy periods, breast tenderness) and lower effectiveness, emergency contraception should not be used as the primary means of contraception.
How it works:
Emergency contraception pills are thought to work through a number of effects mostly by preventing fertilization through disrupting ovulation or interfering with the movement of sperm towards the egg. Depending on what sort of emergency contraception is used, other possible mechanisms include interfering with the corpus luteum or preventing implantation (i.e., they do not seem to cause abortions, rather they prevent fertilization in the first place).
How to Get it:
Most current birth control pills can be used for emergency contraception though only the Preven emergency contraception pill has been approved in the US for use. Call or visit your doctor, health care clinic, or emergency room to learn how to take the medicine or get it prescribed. Click here for a list of local clinics, or call 1-888-NOT-2-LATE for information about method options and provider referral. Emergency Contraceptive Pills (most commonly used): This is a regimen of combined estrogen-progesterone oral contraceptive pills taken within 72 hours of unprotected intercourse. It may cause significant nausea and vomiting.Progestin-only minipills can also be used; they work through a similar mechanism as OCPs and may be more effective than the estrogen + progesterone combinationsCopper IUD insertion is a less common method, but works within 5 days of intercourse and may be 98% effective. Copper ions act to prevent fertilization.
RU-486 (The Abortion Pill):
RU-486 (mifepristone) is an anti-progestin which prevents ovulation and slows maturation of the uterine lining. A single dose of mifepristone has been shown in studies to be effective in preventing pregnancy when given within 72 hours after unprotected intercourse with low incidence of side effects. By suppressing ovulation, it acts to prevent fertilization (RU-486 was licensed for this use in the US on September 28, 2000).RU-486 can be used only within 49 days of the beginning of the woman’s last menstrual period. The woman takes three mifepristone pills. Two days later, she returns to the doctor to swallow a second drug, misoprostol, that causes uterine contractions to expel the embryo. The woman then will return for a follow-up visit within two weeks to be sure the abortion is complete.The FDA will allow mifepristone to be distributed only to doctors trained to accurately diagnose the duration of pregnancy and to detect ectopic, or tubal, pregnancies, because those women cannot receive mifepristone. Also, the FDA restricted mifepristone’s use to doctors who can operate in case a surgical abortion is needed to finish the job or in cases of severe bleeding – or to doctors who have made advance arrangements for a surgeon to provide such care to their patients.Studies show mifepristone is 92 percent to 95 percent effective in causing early abortion, by blocking action of a hormone essential for maintaining pregnancy. Without that hormone, progesterone, the uterine lining thins so an embryo cannot remain implanted and grow. The pill-induced abortion can be painful, causing bleeding and nausea. Heavy bleeding is a potentially serious side effect but one the FDA determined is rare. In safety testing of the first 2,100 American women who took mifepristone, four bled enough to need a transfusion. Listed below are the most common formulations and emergency contraception medications available. Consult your own physician before using any of these medications for this purpose. Common Emergency Contraception Medications
| Brand Name | Formulation | Dosage | Efficacy (estimate) |
| Preven Emergency Contraception Kit | Levonorgestrel 0.25, ethinyl estradiol 50 mcg | 2 tablets initially (within 72 hours of intercourse), repeat (2 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Ovral | Norgestrel 0.30 mg, ethinyl estradiol 50 mcg (white tablets) | 2 tablets initially (within 72 hours of intercourse), repeat (2 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Lo/Ovral | Norgestrel 0.30 mg, ethinyl estradiol 30 mcg (white tablets) | 2 tablets initially (within 72 hours of intercourse), repeat (2 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Levlen, Nordette | Levonorgestrel 0.15, ethinyl estradiol 30 mcg (light-orange tablets) | 4 tablets within 72 hours of intercourse, repeat (4 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Levora | Levonorgestrel 0.15, ethinyl estradiol 30 mcg (white tablets) | 4 tablets within 72 hours of intercourse, repeat (4 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Tri-Levlen, Triphasil | Levonorgestrel 0.125, ethinyl estradiol 30 mcg (yellow tablets) | 4 tablets within 72 hours of intercourse, repeat (4 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Trivora | Levonorgestrel 0.125, ethinyl estradiol 30 mcg (pink tablets) | 4 tablets within 72 hours of intercourse, repeat (4 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Alesse | Levonorgestrel 0.1, ethinyl estradiol 20 mcg (pink tablets) | 5 tablets within 72 hours of intercourse, repeat (5 more tablets) in 12 hours | 75 – 85% of pregnancies prevented |
| Ovrette (progestin-only minipill) | Norgestrel 0.075 (yellow tablets) | Twenty (20) tablets within 72 hours of intercourse, repeat (20 more tablets) in 12 hours | 90% of pregnancies prevented |
| Mifepristone | RU-486, 200 mg | 3 tablets (600 mg dose) one time, followed 2 days later with misoprostol | 92 – 95% of pregnancies aborted |
RESOURCES
There are a wide variety of contraceptive methods you and your partner can choose from to avoid pregnancy and STDs. Sexual decision-making and contraception is an important decision, and one that you and your partner should discuss together in a relaxed atmosphere. It’s always a good idea to talk with your doctor about the choices that may be best for your body and your medical needs. Remember: sex is an important and personal decision for both you and your partner. It can bring about a special bond of closeness and intimacy, but can just as easily bring emotional upheaval, unplanned pregnancies, and sexually transmitted diseases (many of which cannot be cured and may even be deadly).
Other helpful links and further readings are as follows:
Managing Contraception (By Robert Hatcher, M.D.) In addition to this detailed book, an excellent website written by Dr. Hatcher and maintained at Emory University’s Medical School is an excellent and unbiased source for detailed information on almost all contraceptive and emergency contraceptive techniques.
Our Bodies, Ourselves for the New Century: A Book by and for Women (by Boston Women’s Health Book Collective)
In conclusion, communication, honesty, and planning, are crucial in determining whether a sexual relationship is right for you, and if so what form of contraception is best. There are many resources out there to help you make a decision. Your primary care physician (ob-gyn, family practitioner, internist or pediatrician) is an excellent source of advice and counsel. You can also call your local Planned Parenthood office for advice and counseling on contraceptive options. Depending on your religious and personal beliefs, discussion with your priest, rabbi, chaplain, or other spiritual leader may also be helpful in determining the right course of action for you for these important, yet personal, issues.
Other Sources Used: Contraceptive Technology, 17th ed. Hatcher, et al, ed. Ardent Media 1998. “Sex Inc.” Brown Univ. Office of Health Education, 1997 Danakas, GT and Pietrantoni, M. Practical Guide to the Care of the Gynecologic/ Obstetric Patient. Mosby-Year Book, Inc., 1997. Assorted OB-GYN clerkship notes., Managing Contraceptive Pill Patients, 9th ed., by Richard Dickey, MD, Ph.D.
MALE CONDOM
As far back as 1350 BC, there are records of Egyptian men wearing sheaths as decorative covers for their penises. In the eighteenth century, condom use became popular for protection against infections and unwanted pregnancies. The condom is usually made of latex rubber (another name for it is “a rubber”) and is meant to fit an erect penis. Many condoms come lubricated and/or premedicated with spermicide (a chemical that kills sperm cells on contact). Other condoms made of lamb intestines are more expensive and may not protect as well against sexually transmitted diseases. Condoms are designed to keep semen from getting into the woman’s vagina. To maximize the protective benefits of condoms, they must be used correctly.
Condoms usually come rolled up in a package. It will unroll to about 7 1/2 inches, though one should not unroll it until putting it on the erection. A 1 3/8 inch ring is found on the open end to help prevent the condom from slipping off during use. The closed end often has a nipple reservoir that catches semen and helps prevent the condom from breaking. A high-quality latex condom has a failure rate of 1% – 2%, meaning that one can expect their condom to break, burst, contain a minute hole, or slip off, once or twice every 100 times of use. Because of this, only abstinence is completely effective at preventing STDs.
To use a condom correctly, pinch the end (the nipple) to get the air out prior to placing it on the head of the penis. This pinched-off space will be where the ejaculate collects and minimizes the risk of bursting the condom. Roll the condom down the shaft of the erection, covering as much skin as possible (many STDs can spread from skin to skin contact even if there are no open sores or rashes present). The condom must be unrolled onto the erection before any intercourse occurs as it is common to leak a small amount of semen from the stimulated penis prior to ejaculation.
If you are not using a lubricated condom, you should put K-Y Jelly or a spermicide onto the condom once it has been placed on the erection to lubricate and hence minimize the risk of tearing the condom during sexual relations. NEVER use Vaseline (petroleum jelly) on the condom as it can dissolve the latex. When withdrawing the condom-covered penis from the vagina or mouth, be sure to hold the rim to prevent it from slipping off and spilling sperm onto mucous membranes. In case of an accidental spill around or in the vagina, insert spermicide cream, jelly, or foam gently in and around the vagina. Do not douche.
