
Lyme disease was discovered in, and named after, Lyme, Connecticut in the mid-1970s when doctors noted a relatively large number of area children developing arthritis (joint swelling). Doctors soon realized that many of these children lived near wooded tick-infested areas and that their symptoms began during the summer months, coinciding with the height of tick season. Many of those infected reported a target-shaped rash prior to the onset of the joint swelling.
In Europe, the medical literature reports a similar rash and arthritic disease dating back to the 1900s. It is now believed that Lyme disease may have spread from Europe to the United States in the early 1900s but only recently has became widespread enough to be rediscovered.
Currently, Lyme disease is a relatively common illness found throughout the United States but with marked “hot spots” in the Northeast (Massachusetts to Maryland), the Midwest (Wisconsin and Minnesota), and the West (California). It is one of the many diseases caused by tick bites (so called tick-bourne infections).

Though spread by the deer tick, Lyme disease is actually caused by the bacteria, Borrelia burgdorferi (pictured as seen under a microscope). This bacteria is found in approximately 20% of all deer ticks. If an infected deer tick (not to be confused with the more common dog tick) bites you, your chances of getting Lyme disease are perhaps 10% or less (depending on how long the tick has been feeding on you). Prompt removal of the deer tick significantly reduces your chance of getting this disease. In fact, it is quite unlikely that you will get Lyme disease if the tick is removed within 1 – 2 days of attaching to you. Unfortunately, because the deer tick is often found in its “nymph”, or baby, state, it is often not even noticed on the skin. The American Lyme Disease Foundation warns that in addition to Lyme disease, two more tick-borne diseases are also on the rise: Ehrlichiosis (Human Granuloctic Ehrlichiosis, HGE) and babesiosis. These are carried by the same species of ticks that cause Lyme disease, namely the Ixodes species. HGE is most often found along the East Coast and in the Midwest. General symptoms are high fever, headaches, and vomiting. Symptoms for babesiosis occur approximately one to two weeks after being infected. A gradual fatigue takes over, followed by fever, sweating, headaches, and muscle pain. Babesiosis occurs on both the East and West Coasts. Lyme disease, Babesiosis, and Ehrlichiosis, are all spread by the species of tick called Ixodes (deer tick). These ticks are smaller than the common “dog tick”. Other tick-bourne diseases include Rocky Mountain spotted fever, tularemia, and relapsing fever.

TICK LIFE CYCLE
The life cycle of a tick can be classified into 4 stages.
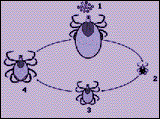
Ticks are relatives of spiders, scorpions, and mites. As such, their survival is dependent on a host (i.e., they’re parasites). Specifically, ticks feed on an animal’s blood or body fluids. The deer tick (Ixodes scapularis in the East & Midwest, and Ixodes pacificus in the West) goes through many stages during its lifecycle, and feeds on different species at each point.
Ticks begin as eggs (stage 1) that hatch into 6-legged larvae (stage 2).
Larvae live and feed on animals (mice, deer, squirrels, livestock, and any humans who enter the tick habitat) for about a week before detaching then molting (shedding) anywhere from 1 week to 8 months later.
The larvae then become 8-legged nymphs (stage 3). Nymphs feed on animals, engorge for 3 to 11 days, detach, and molt about a month later (depending on the species and environmental conditions).
Once the nymph molts, it becomes an adult tick (male or female). Ticks climb up grass and plants and hold their legs up “sensing” and “looking” for their prey. Ticks are attracted to their hosts by detecting carbon dioxide and heat through special organs located on the first pair of the tick’s legs (Haller’s organs). When a warm-blooded animal walks past, the tick can crawl onto them and begins feeding. Ticks insert their mouths, attach to their prey, and engorge themselves with a blood meal (stage 4). During feeding, tick saliva can get into the host’s body and blood stream. Any tick infected with Borrelia burgdorferi can then inadvertently spread this bacteria to the host.
Male and female ticks usually mate while attached to the host. A few weeks later, the engorged female detaches from the host and lays her eggs (1000 – 8000 eggs) on a leaf. A tick usually lives a year before dying.

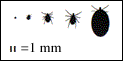
SIGNS & SYMPTOMS
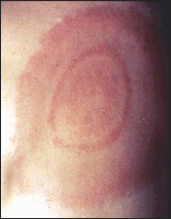
The first sign of Lyme disease is often a rash. Though it can take on many different appearances, the rash usually resembles a bulls-eye and is warm to the touch. This rash, called erythema migrans (EM), occurs in 75% of those infected with Lyme disease. The EM “bulls-eye” rash appears 3 to 30 days after getting the tick bite, and often is accompanied by fever, joint aches, and other flu-like symptoms.
Within days of infection, the bacteria can spread throughout the blood stream often causing rashes at other sites (see last picture below of multiple rashes on a woman’s legs). Often this spread of Lyme causes high fever, headache, chills, muscle aches, joint aches, and profound fatigue. All these symptoms usually go away in several weeks, even without treatment.
Unfortunately, if your Lyme disease isn’t treated, it can come back anywhere from weeks to months later. Secondary and tertiary Lyme disease (as this recurrent Lyme is called) is much more serious as the bacteria can infect your many body systems, including heart, nerves, and joints. Symptoms include cardiac problems such as inflammation of the heart (carditis), neurologic problems such as bell’s palsy or meningitis, and musculoskeletal problems such as painful swelling of the joints (arthritis). Many other symptoms and signs have been attributed to Lyme disease.
TREATMENT
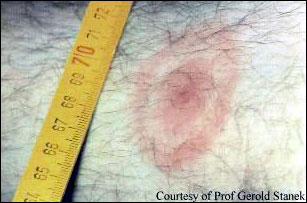
Diagnosis of Lyme disease is based on your symptoms and physical signs. For example, if you have had a deer tick bite, and now have the erythema migrans rash (pictured), you most likely have Lyme and should certainly be treated with an antibiotic.
Blood tests may help with the diagnosis in some instances (i.e., if you never got or don’t remember getting the rash, or if your symptoms are not straightforward). But blood tests are not mandatory and may be falsely negative or positive.
As a bacterial disease, Lyme is treated with antibiotics (e.g., doxycycline, amoxicillin, cefuroxime, and clarithromycin are commonly prescribed). Studies have shown that two to four weeks (and sometimes more) of antibiotic treatment are needed to kill the Borrelia burgdorferi bacteria that causes Lyme. For severe Lyme disease (such as carditis or meningitis), antibiotics given intravenously are often necessary.
If you think you have or had untreated Lyme, you should see your physician to discuss your concerns.
PREVENTION
Prevention is the best strategy for avoiding Lyme disease. To reduce tick bites, avoid tick-infested areas like fields, tall grass, bushes, and woods. If you must go into these areas, wear light-colored long pants and a long-sleeve shirt. Tuck your shirt into your pants, and your pant legs into your socks. Sure, you may look a bit silly, but avoiding this infection is worth the teasing of your family and friends.
As a tick repellent, use an EPA approved DEET-containing product with 20 – 30% DEET as directed on the label. Though a good product, DEET should be used with caution as it is absorbed through the skin. It is best to use DEET sparingly and on clothing instead of skin, if possible. Avoid inhaling or ingesting DEET, and avoid using it on sunburns, cuts, or other damaged skin. Be particularly careful with DEET on children, and don’t use this chemical on infants.

When returning indoors, do a full body inspection (with and without your clothes) to be sure there are no ticks on you or your pets. Also, wash off any chemical repellent with soapy water.
Be sure to check your pets, as cats and dogs commonly carry ticks from their habitat to yours. Pets can easily catch Lyme disease as well. Warning signs in pets include a fever, poor appetite, intermittent lameness, and one or more swollen, warm, and painful joints. Using a tick repellent such as Frontline monthly on your pet will markedly decrease your pets risk of catching this illness.
Summary of Lyme Prevention:
1. Avoid tick habitats (tall grass, bushes, brush, and woods).
2. Dress properly if you must go into a tick habitat.
3. Check for and remove ticks on yourself or family members as soon as possible after leaving a tick habitat.
4. Check pets for ticks and use tick-control pet products.
5. Consider getting vaccinated if you live in an area with a lot of Lyme disease.

COMMON QUESTIONS
I heard there is a Lyme vaccine. How, and should, I get one?
A vaccine for Lyme disease, called LYMErix, is now available. LYMErix is given in a 3 shot series at 0, 1, and 6 to 12 months. Studies have shown that after the series, 78% of those immunized were protected against Lyme disease. The vaccine is currently approved for those aged 15 through 70 years old. Recently, however, there has been some concern that the vaccine may cause arthritis-like symptoms. Therefore, it makes sense only to get the immunization if you live in an area with a very high risk of Lyme disease AND if you are commonly in fields and woods where you will likely be exposed to deer ticks.
A large study is currently underway to determine if this vaccine will be safe and effective in children aged 4 and older. Your doctor can give you more information on who should be vaccinated, but those who often are exposed to tall grass and fields, and in an area where lyme is prevalent should strongly consider being vaccinated.

There’s a tick on me! What do I do?
If the tick is attached, use a fine-point tweezers to pull the tick off gently by its mouthparts. Grasp the tick with the tweezers as close to your skin as possible and with a gentle, yet firm upward motion, pull the tick out. Don’t pull it off by its belly as you might squeeze infected fluids into your skin by mistake. Also, don’t try to burn or crush the tick for the same reason, as the tick may regurgitate into the bite. Smothering the tick with petroleum jelly or nail polish often doesn’t work fast enough, and the tick often has enough air to finish its meal (and infect you).
Once removed, wash your hands, the tweezers, and the bite site with warm soapy water. Keep watch for a rash or skin infection, and alert your doctor if you have any questions or concerns, or if you develop a fever or illness.

Remove ticks by grasping as close to your skin as possible.
I got the tick off. Should I take antibiotics, or at least get a blood test?
Because the risk of getting Lyme from a deer tick bite is so low (estimated to be less than 1 in 10 people if the tick was attached less than 72 hours), antibiotics are not indicated. In fact, the potential risks of taking unnecessary antibiotics (e.g., allergic reaction, diarrhea, and bacterial resistance) may be just as serious as Lyme disease. Likewise, getting a blood test if you don’t have any symptoms is not necessary. The blood test often won’t show the infection in the first 3 weeks, or it may be falsely negative or positive. If you develop a rash or other flu-like symptoms, you should see your family doctor to see if you have Lyme or another illness.
A recent study showed that taking one dose of Doxycycline antibiotic after a deer tick bite, can significantly decrease the risk of getting Lyme disease. This study showed that without taking the antibiotic, you have a 3.2% risk of catching Lyme disease after a deer tick bite. Taking one dose of antibiotic reduced the chance of Lyme by 87%. Based on this, 40 people who had a deer tick bite would have to be treated to prevent just 1 case of Lyme, and since Lyme is fairly easily treated once diagnosed, it is generally not recommended that everybody who is bitten by a deer tick get a dose of antibiotic. (That said, if you live in an area with a lot of Lyme, and you find an engorged deer tick on you, the risk of Lyme is higher (about 10%) and it perhaps make sense to take one dose of Doxycycline (within 72 hours of tick bite). We suggest you discuss this with your doctor.
I’m always tired, should I get a Lyme test?
Many people feel tired or fatigued. It is rare for this to be due to Lyme disease without other symptoms (such as fever, rash, chills, or arthritis). If you feel chronically exhausted, it is important to see your family doctor to discuss more common causes of this problem, like depression, fibromyalgia, or thyroid abnormalities. In addition to a thorough history and exam, blood tests to look for anemia, thyroid disease, and possibly Lyme disease might be considered.
RESOURCES

This online guide has discussed the many aspects of Lyme disease, including the causes, symptoms, diagnosis, and treatment. We hope you have found our online guide helpful and informative. There are a number of good sources for information on Lyme and other tick-bourne diseases.
Your family physician can often answer your medical questions, and is a great resource. The Lyme Disease Foundation has a website with good links and other materials (800-886-LYME). To get verbal instructions on removing ticks and other Lyme disease info, call 1-888-SCH-TICK.
For more in-depth analysis on Lyme and infectious diseases in general, these texts are helpful.
Everything You Need to Know About Lyme Disease and Other TickBorne Disorders (by K. Vanderhoof-Forschner)
LYME MAPS
FIGURE 1. World locations of recognized Lyme disease
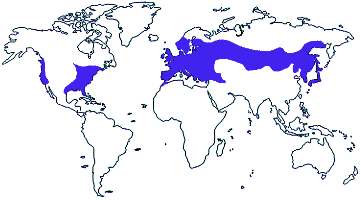
FIGURE 2. Number of reported cases of Lyme Disease per year in the United States
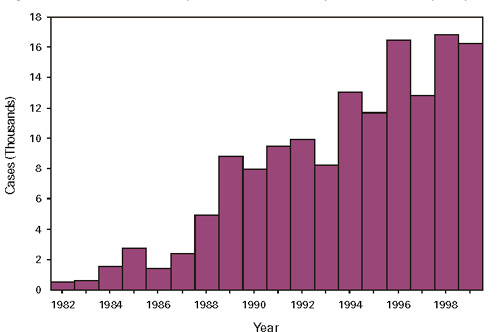 FIGURE 3. Number of reported cases of Lyme Disease by County, 1999 FIGURE 3. Number of reported cases of Lyme Disease by County, 1999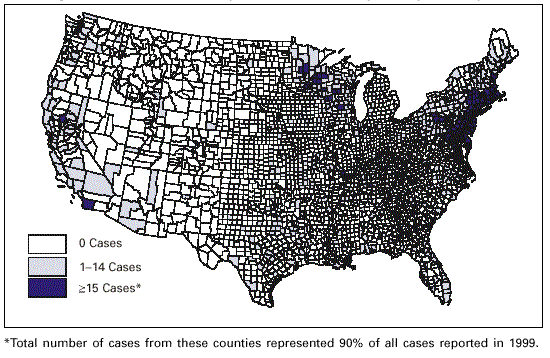 |
STAGES
Stage 1 (primary Lyme disease)
Stage 2 (secondary Lyme) – days to weeks after untreated primary Lyme
Stage 3 (tertiary Lyme) – months to years after untreated primary Lyme
Even more problems reportedly associated with Lyme disease (Borrelia burgdorferi) infection. Please note, not all of these have been proven to be caused by this infection and may be due to other diseases. |
|||||||||
|
